A day in the life of an…orthoptist!
Gaëla Cariou-Panier always knew she wanted to work in healthcare. She even loved the smell of hospitals. After two years of medical school in France and some time working in research, she came across a job she had never heard of: orthoptist. “It was a hard word to say,” she laughs. “But as soon as I learned more about it, I knew it was for me.”
What’s an orthoptist?
Orthoptists specialize in evaluating, diagnosing and treating patients who have crossed eyes, double vision or lazy eyes. The majority of these problems are congenital and are due to a weakness or paralysis of an eye muscle. “Our goal is to find out which muscle or nerve is affected, how long has this been going on for, why, and how can we treat it?” explains Gaëla. “We work closely with the ophthalmologists. More often than not, we see patients with strabismus first, in order to give the diagnosis and determine if an operation is necessary.”
Their main objective is to straighten the eye, strengthen the weaker eye, or refer to surgery if none of the treatments help and prescription glasses don’t work. Most of their patients are treated by various non-surgical treatment options, like glasses and/or wearing a patch over the dominant eye in order to strengthen the weaker one. However, a quarter of their patients have a more complicated reason behind their visual impairment, like a brain tumor.
Small team, big results
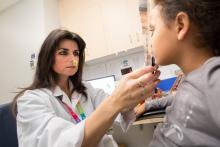
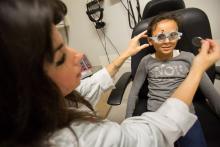
There are three orthoptists at the Montreal Children’s Hospital, Gaëla, Mona Hijazi and Stephanie Oglietti. They each see approximately 12-13 patients a day and a consultation can last between 20 to 45 minutes. During a regular appointment, Gaëla will observe, measure and use different techniques, like using a prism to determine the gravity of the problem. A prism is an optical device that can be placed on a patient’s glasses to trick the brain into thinking that the eyes are straight. The strength of the prism can be easily adjusted until the eye is recentered and the prism is then removed.
During a consultation, Gaëla will check a patient’s 3D vision, as well as the muscles around the eye. “We have six muscles in each eye that allow it to move and I can figure out which muscle is not working by simply looking at it,” she says. The eye will drift outward, inward, upward or downward depending on which muscle is affected. If there is any deviation, she figures out which muscle is not working and then measures the angle of the deviation. “These measurements help the ophthalmologist with the surgery,” she says.
Time is key
Time is crucial in a lot of these cases, because the younger the child, the better chance they have of solving the problem. “A patch will be more effective with children under six and a half years old, because after that the visual function matures and recovery is more difficult,” she explains. This tight time frame is important when explaining to parents why they have to be vigilant with this treatment option. “Even if it takes me five extra minutes, I always explain why it’s important for their child to wear the patch,” she says. “If they understand the ‘why’ then they will more likely go home and make sure their child wears it.”
Clowning around
A lot of their patients don’t speak yet so they use special instruments, toys and techniques to try and figure out if these children can see properly or not, and each of the orthoptists do it in a different way. For Gaëla, she likes to clown around. “I love being a clown and using my humour during consultations. I’ll stick things on my nose so they can focus on one thing or I’ll let them watch TV to calm them down while I take a closer look at their eyes.”
As a mother of two teenage girls, she understands what these parents are going through and tries to help them navigate these difficult times by making them laugh and smile. “If it’s appropriate, I will ask the parents to participate in our little games and I even get the child’s stuffed animal involved too,” she laughs. “I’ll either put drops in their eyes or send their teddy bear home with a patch!”
In high demand
It is very evident that Gaëla’s job is not just a job – it’s her passion; a passion that she also gets to share with adult patients as well. Orthoptists are in very high demand so they often work in pediatric and adult settings. In fact, the Programme d’Intégration Francophone des Orthoptistes (PIFO) was put into place in order to allow francophone orthoptists, like Gaëla, to work in Canadian hospitals. “We have over 2,000 orthoptists in France, but only 20 to 30 in Quebec,” she says. “It was a no brainer to move here for a job I love.”
“I always tell my daughters it’s important to wake up in the morning and love what you do. I love my job because it varies enormously every day. Even if the pathology looks similar, the patient is always different. Orthoptists don’t treat the cause; we solve the problem.”