Dispatches from the Africa Mercy #5: It Takes a Mercy Ship
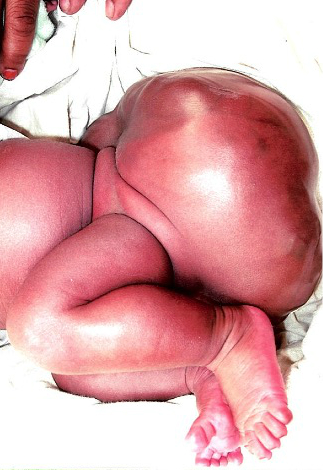
March 8, 2016 18:30: Today marks the sixth day after Polly’s operation. She is looking better and better, brighter and brighter. She is her mother’s child but she is also the child of the Africa Mercy, a testimony to the power of this Ship. (Photo left: Polly before the surgery).
The baby is identified by Mercy Ships during one of their screenings far from Tamatave. I find out about her before arriving on the Ship. Mirjam, the screening coordinator, sends me her pictures, hoping that a pediatric surgeon might be able to help.
I open the file in my office at the Children’s to a moment of disbelief. The baby has a rare tumor called a sacrococcygeal teratoma, larger than any I had ever seen. She was born in November, and continues to grow and thrive despite this massive tumor on her back, approximately twice the size of her head. I ask Mirjam to get some imaging done, which is accomplished by the Ship’s radiology technician, and sent to a radiology group in Canada to be read. I receive the report days before I leave for Madagascar. There are no convincing reasons not to attempt removal of this tumor, which will eventually turn malignant, and take her life.
Days later, I am face to face with Polly and her mother. I review the imaging and examine the baby. She is beautiful, and it hurts to see her mother struggling to hold her due to the mass, which is now even larger and essentially obliterates her buttocks and lower back. But it is still removable. I discuss the surgery and all its potential complications with Polly’s mother. She has no questions. This is the day she has been waiting for since the baby’s birth.
The Africa Mercy operates at a very high level of accountability and responsibility. The Ship is not an acute care hospital. It does not manage major pediatric congenital anomalies early in life. No such tumors had been previously resected on the Ship. The case therefore has to be reviewed by a hospital board, in order to decide whether to take it on. The main concerns are whether this could be done safely and whether the child has a high chance of disabilities that cannot be managed after the Ship’s departure. I point out that this child has already proven her desire to live. She was delivered vaginally without rupture or hemorrhage from the tumor, and has thrived and grown despite it. A decision is made to proceed. Together with anesthesia and nursing, we plan every step.
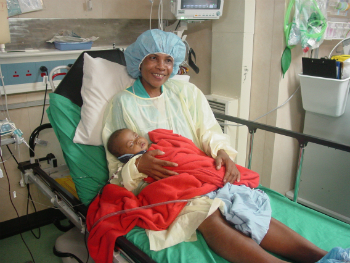
On the day of surgery, I start with placing a central venous line in a large vein draining into the heart to give us good access if we encounter bleeding. We proceed slowly and deliberately with the operation, one small step at a time. Three hours later, the tumor is out, and Polly has been stable the entire time. We extubate her and send her to the recovery room, where her mother will see her for her first time without the monstrous deformity. (Photo right: Polly with her mother in the recovery room after the surgery).

That night, as I head to dinner, I experience the power of the Africa Mercy community. The food servers and cooks, who have nothing to do with the operating room, ask me how the surgery went. In response to my puzzled look, they tell me that their entire team prayed for her as she was heading into the operating room. This experience is repeated throughout the evening as many residents of the Africa Mercy, who I do not work with and had not met, approach me to ask about Polly and reassure me that they will continue to pray for her recovery.
In the ensuing days, their prayers are answered. Polly is in a ward of 12 patients sharing a single large room. The other patients and families rally around her. The nurses take impeccable care of her, attending to her almost hourly to keep the wound clean and dry. On the second day, the drain in Polly’s buttocks is removed. On the third day, her bladder catheter is removed, and her bladder starts to function normally. Today, her biggest challenge is to satisfy the wishes of all the nurses who want to cuddle her.
What does it take to see hundreds of patients like Polly safely through deforming diseases and severe anomalies? It takes screening throughout the host country, linking the patient with the appropriate surgeon, transporting the patient and mother to the port city, performing the needed imaging, hosting the patient in the port city for several weeks pending the surgeon’s arrival, planning responsibly to perform the case safely, providing excellent nursing care, and having an entire community of 420 crew from 36 countries support the mission in faith and prayer. It takes a Mercy Ship. (Photo left: Polly with Deborah, her French ward nurse, 5 days after the surgery).
 Dr. Sherif Emil is a pediatric surgeon and Director of the Division of Pediatric General and Thoracic Surgery at the Montreal Children's Hospital. Over the 2 weeks, he will be part of the volunteer crew of the Africa Mercy, currently docked in Tamatave, Madagascar. The Africa Mercy is the world's largest civilian hospital ship dedicated to bringing hope and healing to tens of thousands of the world's impoverished populations.
Dr. Sherif Emil is a pediatric surgeon and Director of the Division of Pediatric General and Thoracic Surgery at the Montreal Children's Hospital. Over the 2 weeks, he will be part of the volunteer crew of the Africa Mercy, currently docked in Tamatave, Madagascar. The Africa Mercy is the world's largest civilian hospital ship dedicated to bringing hope and healing to tens of thousands of the world's impoverished populations.
Read more:
Dispatches from the Africa Mercy # 1: The End of the Earth
Dispatches from the Africa Mercy # 2: Can it get any better?
Dispatches from the Africa Mercy #3: The Heroes of Africa
Dispatches from the Africa Mercy #4: The Power of Camaraderie
Dispatches from the Africa Mercy #6: Jane
Dispatches from the Africa Mercy # 7: A Vision of Mercy (Final Dispatch)


